Tailbone Pain (Coccydynia)
Tailbone Pain (Coccydynia) Treatment Starts Here
Tailbone pain—also called coccydynia—can make sitting, driving, and moving from sitting to standing uncomfortable. It often follows a fall or prolonged sitting, but it can also develop gradually. At Mountain View Pain Center, we help identify what’s driving your symptoms and build a plan to reduce pain and restore comfortable daily activity.

Common Symptoms of Tailbone Pain
Pain at the tailbone, especially when sitting
Pain that worsens with leaning back in a chair
Discomfort with transitioning from sitting to standing
Pain with prolonged driving
Tenderness over the tailbone area
Pain that can flare with bowel movements
Symptoms that improve when standing or using pressure relief
Bruising/soreness after a fall or direct impact (when injury-related)
Common Causes and Risk Factors
Fall or direct impact to the tailbone
Prolonged sitting on hard surfaces
Repetitive strain (cycling/rowing or similar seated activities)
Childbirth-related strain
Pelvic floor tension or muscle imbalance
Joint irritation or abnormal tailbone mobility
Degenerative changes over time (less common)
Weight changes (either loss of cushioning or increased pressure)
When to Seek Urgent Care
Seek urgent evaluation if you have severe pain after trauma with inability to sit or walk, fever/chills, unexplained weight loss, new numbness/weakness, loss of bowel or bladder control, or rapidly worsening symptoms.
How We Evaluate Tailbone Pain
Tailbone pain can have several causes, so we start by clarifying your history, symptom triggers, and sitting tolerance. Your visit may include assessment of posture, pelvic alignment, hip mobility, and surrounding muscles. We also check for red flags and consider whether imaging or referral is appropriate—especially after significant trauma or if symptoms persist.
How We Treat Tailbone Pain
At Mountain View Pain Center, our multidisciplinary team combines evidence-based care to reduce irritation and improve pelvic stability:
Pain Management
Targeted diagnostic injections and image-guided procedures when appropriate to reduce inflammation and calm irritated tissues.
Physical Therapy
Movement-based care focused on pelvic/hip mobility, core stability, and strategies to improve sitting tolerance.
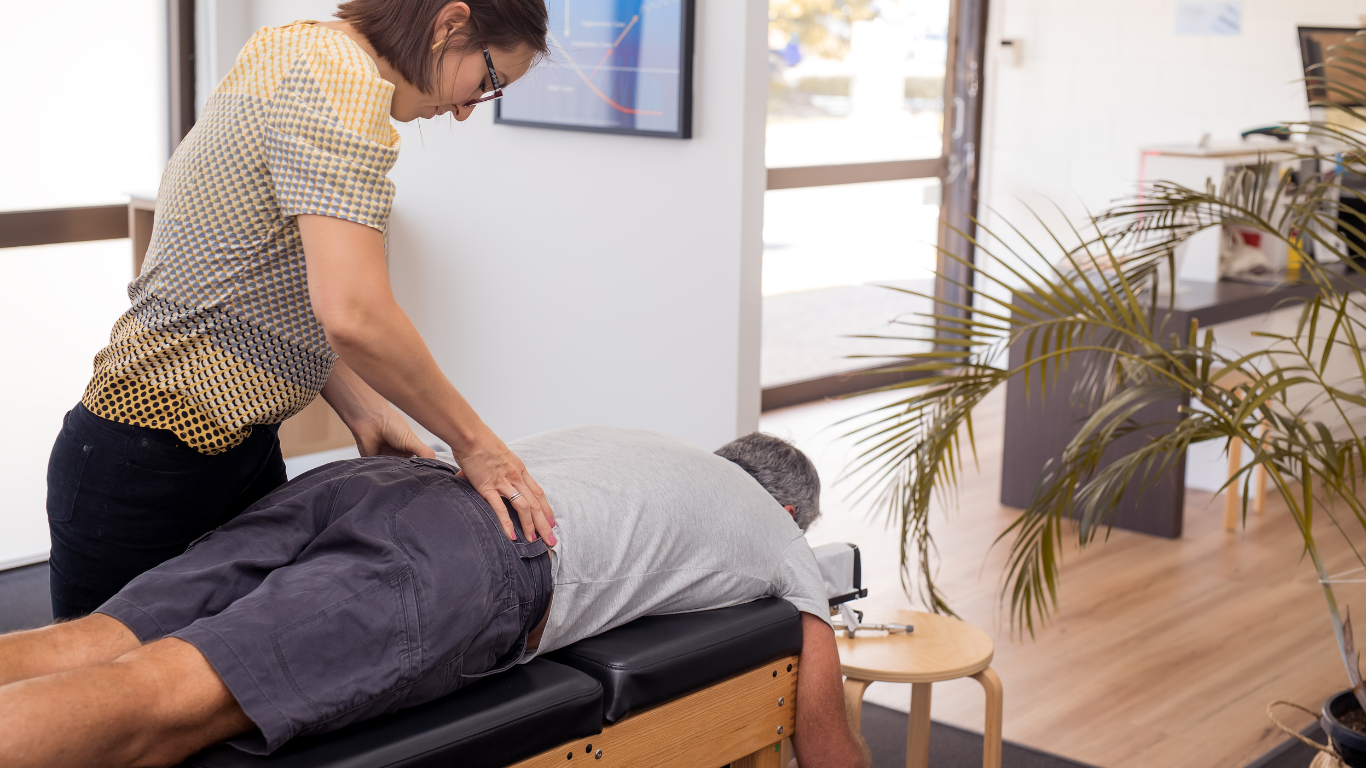
Chiropractic Care
Hands-on care to support mobility and reduce muscle tension, tailored to your symptoms and comfort.
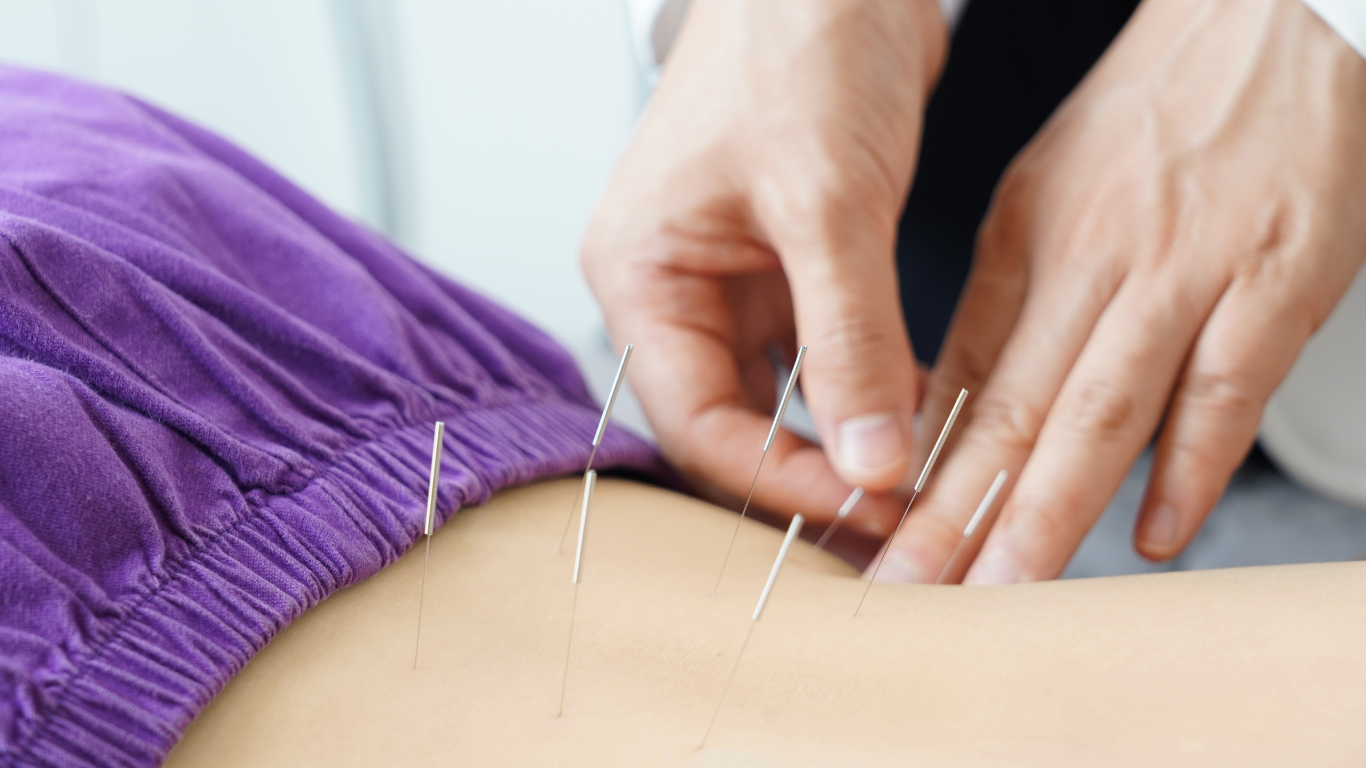
Acupuncture
A natural option to support pain relief and relaxation, often combined with your broader plan.
Treatments We Commonly Recommend
Sitting tolerance strategies and posture coaching
Hip and pelvic mobility work
Core and glute strengthening to support pelvic stability
Manual therapy to reduce muscle tension
Graded return-to-activity plan
Image-guided injections (when appropriate)
Home program to reduce flare-ups and build consistency
Home Care & Quick Relief
Ice for 10–15 minutes at a time, especially during flare-ups
Limit prolonged sitting; take frequent standing/movement breaks
Use a pressure-relief cushion (donut or wedge cushion) when sitting
Avoid leaning back into the tailbone—try upright posture and gentle position changes
Stay gently active (short walks) as tolerated
Tailbone Pain FAQs
-
Coccydynia is pain around the tailbone, often worse with sitting or transitioning from sitting to standing.
-
It depends on the cause. Some cases improve in weeks, while others take longer—especially if symptoms have been present for a while. Our goal is to reduce pain and improve sitting tolerance with a clear plan.
-
Not always. If pain followed significant trauma or symptoms persist, imaging may be considered. We’ll help guide the next step if appropriate.
-
Many patients do best with a pressure-relief cushion, frequent position changes, and avoiding leaning back into the tailbone.
-
Many people improve with coordinated care focused on mobility, stability, and sitting tolerance—often combining PT, chiropractic care, acupuncture, and, when appropriate, pain management procedures.
-
Often, no. Some insurance plans require a referral or authorization—if you’re unsure, we can help verify.