Post-Herpetic Neuralgia
Post-Herpetic Neuralgia Treatment Starts Here
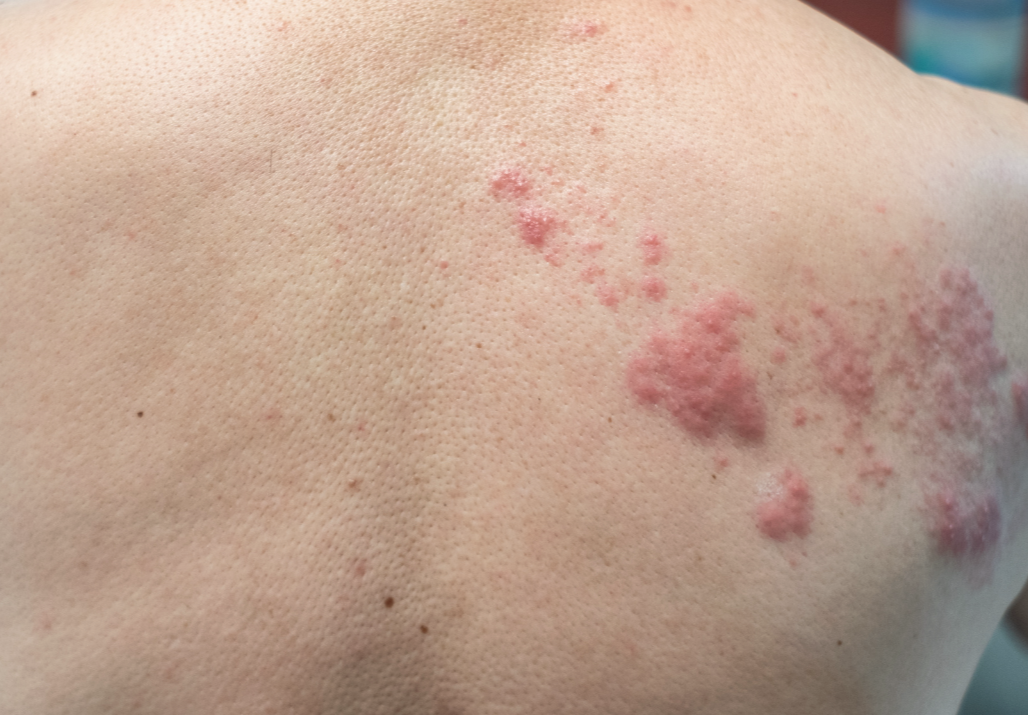
Post-herpetic neuralgia (PHN) is lingering nerve pain that can persist after a shingles infection. Even after the rash heals, some people experience burning, stabbing, or highly sensitive pain in the same area. At Mountain View Pain Center, we help evaluate your symptoms and build a plan focused on pain relief, function, and quality of life.
Schedule Post-Herpetic Neuralgia Relief Today
Common symptoms of post-herpetic neuralgia
Burning, stabbing, or shooting pain in a specific area
Pain in the same region where a shingles rash occurred
Extreme sensitivity to touch (clothing, sheets, light contact)
Itching, tingling, or numbness in the affected area
Pain that worsens at night or with stress/fatigue
Episodes of electric-like “zaps”
Sleep disruption due to discomfort
Ongoing tenderness long after the rash has healed
Causes & contributing factors
Nerve irritation/damage following shingles
Higher risk with increasing age (common risk factor)
Severe shingles pain during the initial outbreak (can increase risk)
Delayed treatment of shingles (sometimes discussed as a contributor)
Stress and poor sleep can amplify nerve sensitivity
Sensory changes that persist even after skin appearance returns to normal
When to Seek Urgent Care
Seek urgent evaluation if you have sudden one-sided weakness, facial droop, slurred speech, severe headache, sudden loss of balance, or rapidly worsening symptoms. If you have reduced sensation plus new wounds, spreading redness, drainage, or signs of infection, seek prompt medical evaluation.
How We Evaluate Post-Herpetic Neuralgia
We start by confirming the timeline of shingles symptoms and where pain persists. Your visit may include a review of pain pattern, sensitivity, and how symptoms impact sleep and daily activity. Because PHN follows a distinct pattern, evaluation typically focuses on symptom history, functional impact, and screening for red flags or other causes if anything is atypical. If additional testing or referral is appropriate, we’ll guide the next steps.
How We Treat Post-Herpetic Neuralgia
Care is tailored to your symptom severity and goals, with a focus on comfort, safety & function.
Pain Management
Options to help manage nerve-related pain and improve day-to-day comfort when appropriate.
Physical Therapy
Movement and conditioning strategies to maintain function, reduce guarding, and support activity tolerance when pain leads to reduced movement.
Chiropractic Care
Hands-on care to support mobility and reduce contributing tension patterns, tailored to your comfort and symptom sensitivity.
Acupuncture
A supportive option that may help reduce discomfort and improve relaxation as part of a broader plan.
Treatments We Commonly Recommend
Strategies to reduce sensitivity triggers (touch/friction management)
Gradual return-to-activity plan to avoid deconditioning
Sleep-support strategies when pain flares at night
Relaxation/stress reduction support (often helpful for nerve sensitivity)
Symptom management plan tailored to your goals
Home Care & Quick Relief
Ice for 10–15 minutes at a time if it helps reduce discomfort
Avoid friction triggers when possible (soft clothing, gentle fabrics)
Use pacing: break tasks into smaller chunks during flare-ups
Gentle movement as tolerated to avoid stiffness and deconditioning
Aim for consistent sleep routines (night flares are common)
Post-Herpetic Neuralgia FAQs
-
It’s nerve pain that persists after shingles. Pain can continue even after the rash resolves.
-
It varies. Some people improve in months, while others have longer-lasting symptoms. Our goal is symptom relief and improved quality of life.
-
PHN itself isn’t contagious. Shingles comes from reactivation of the chickenpox virus; your medical team can advise on contagious periods during an active rash.
-
PHN can cause nerves to become hypersensitive, so light contact (clothing, sheets) may feel painful.
-
Many patients benefit from a coordinated symptom management plan that may include pain management options and supportive therapies to improve comfort and function.
-
Often, no. Some insurance plans require a referral or authorization - if you’re unsure, we can help verify.
Find Post-Herpetic Neuralgia Treatment Today
Related Resources
Related Conditions
Neuropathies
Trigeminal Neuralgia