Myofascial Pain Syndrome
Myofascial Pain Syndrome Treatment Starts Here
Myofascial pain syndrome is pain that comes from irritated muscles and the connective tissue around them (fascia). It often involves tender “knots” or trigger points that can refer pain to other areas—such as the neck, shoulders, upper back, or low back. At Mountain View Pain Center, we help identify what’s driving your symptoms and build a plan to reduce pain, restore mobility, and improve function.

Schedule Myofascial Pain Relief Today
Common Symptoms of Myofascial Pain Syndrome
Deep, aching muscle pain
Tender trigger points or “knots”
Referred pain (pain felt in a different area than the trigger point)
Muscle tightness and reduced range of motion
Pain that worsens with stress, poor sleep, or prolonged posture
Headaches related to neck/shoulder tension
Jaw or facial tension
Fatigue or a heavy feeling in affected muscles
Pain with repetitive activity or prolonged sitting/standing
Common Causes and Risk Factors
Repetitive strain or overuse
Prolonged sitting, screen time, or poor ergonomics
Muscle imbalances and weakness leading to compensation
Old injuries that changed movement patterns (whiplash, shoulder injuries, back flare-ups)
Reduced activity or deconditioning
Stress and poor sleep (can amplify muscle tension and pain sensitivity)
Limited mobility in the neck, shoulders, hips, or upper back
High training load or sudden increase in activity
When to Seek Urgent Care
Seek urgent evaluation if you have severe unrelenting pain after trauma, fever/chills, unexplained weight loss, new or worsening weakness, loss of bowel/bladder control, or rapidly worsening numbness/tingling.
How We Evaluate Myofascial Pain Syndrome
Myofascial pain can overlap with joint or nerve issues, so we start by clarifying your symptom pattern and triggers. Your visit may include movement testing, posture assessment, and evaluation of muscle tenderness and trigger point patterns. We also assess surrounding joints and mechanics (neck, upper back, shoulders, hips) that can contribute to repeated muscle strain. If symptoms include radiating pain, numbness, tingling, or weakness, we may also perform a basic neurologic screen. We also check for red flags to determine whether imaging or referral is appropriate.
How We Treat Myofascial Pain Syndrome
At Mountain View Pain Center, our multidisciplinary team combines evidence-based care to reduce muscle irritation and improve movement:
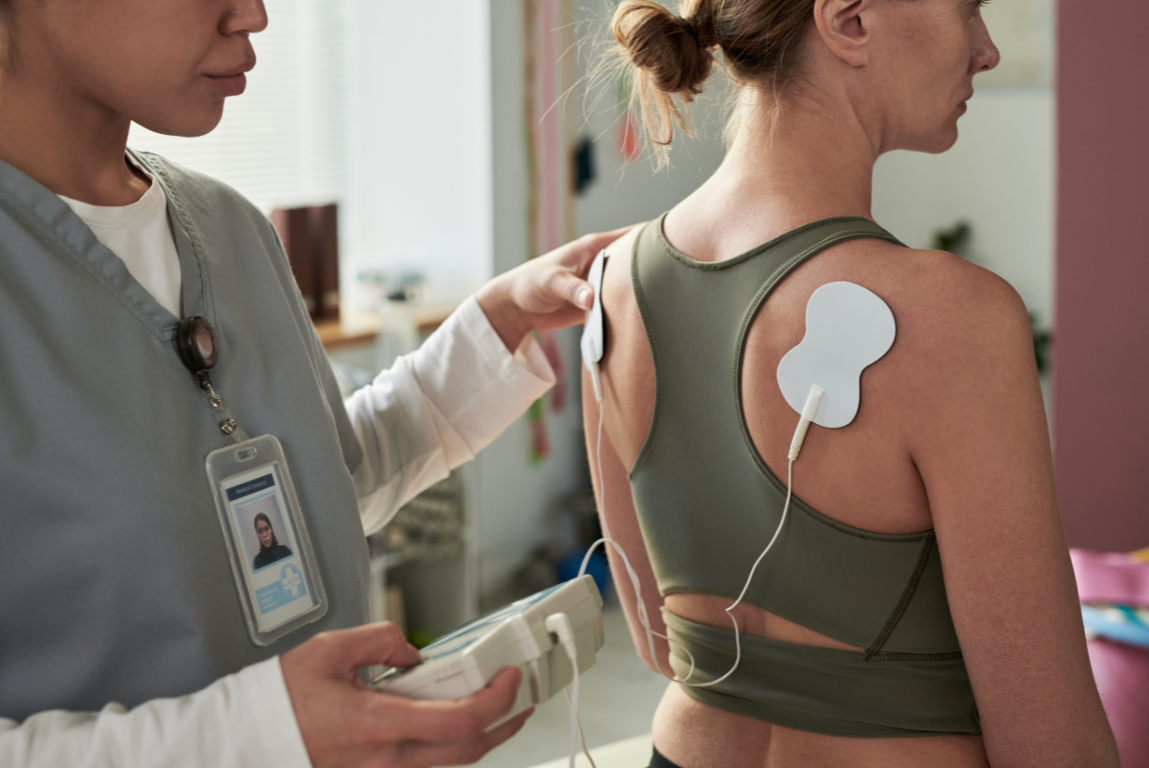
Pain Management
Targeted treatments when appropriate if symptoms overlap with joint or nerve irritation, or if trigger point injections are clinically indicated.
Physical Therapy
Movement-based care to restore neck and upper back mobility, improve strength and stability, and reduce headache/tension patterns.
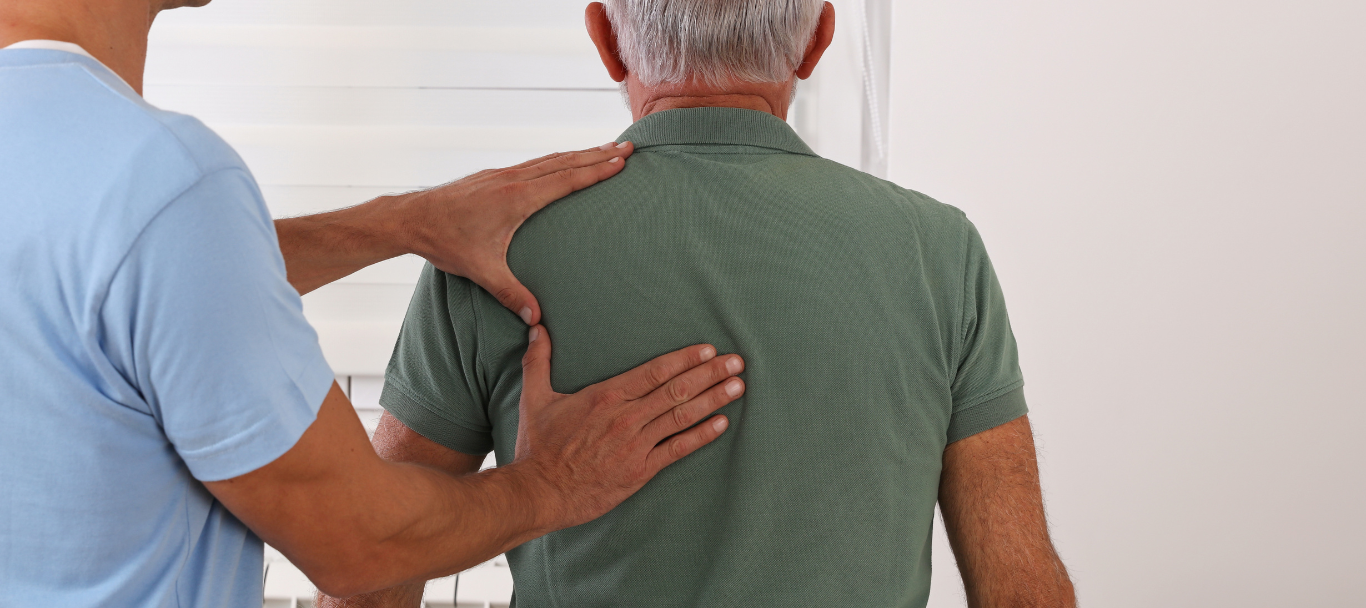
Chiropractic Care
Hands-on care to support joint mobility and reduce muscle tension, tailored to your symptoms and comfort.
Acupuncture
A natural option to support pain relief and relaxation—often helpful for muscle tension patterns and stress-related flare-ups.
Treatments We Commonly Recommend
Trigger point-focused soft tissue work and mobility strategies
Strengthening for posture and endurance (upper back, core, glutes)
Movement retraining for desk work, lifting, and daily habits
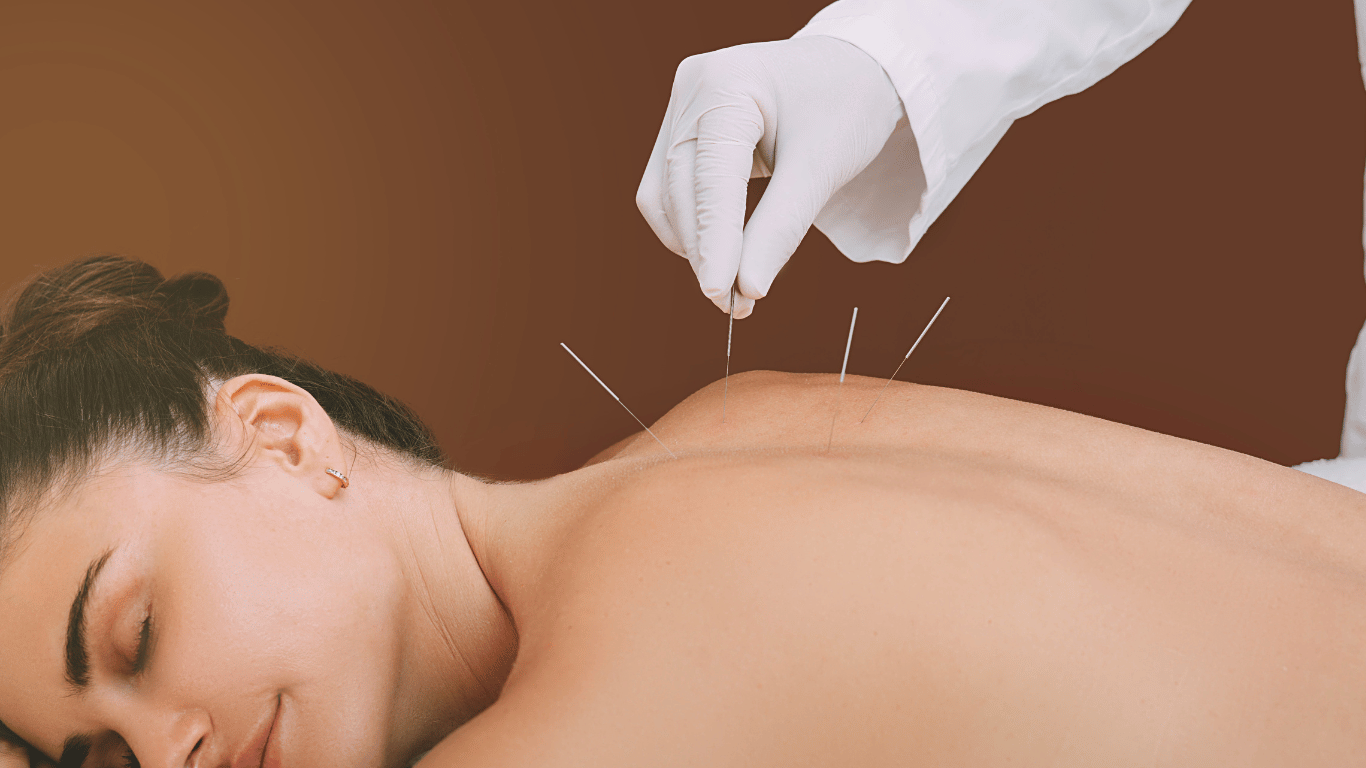
Dry needling
Cupping
Stress/sleep habit support and flare-up planning
Home program to reduce recurrence and improve consistency
Home Care & Quick Relief
Ice for 10–15 minutes at a time during flare-ups
Gentle movement and posture breaks (avoid holding one position too long)
Light stretching and mobility as tolerated
Gradual strengthening for the areas that fatigue easily
Improve sleep consistency when possible (poor sleep often worsens flare-ups)
Myofascial Pain Syndrome FAQs
-
Trigger points are tender, irritated spots in muscle that can cause local pain and referred pain to other areas.
-
Not always. Myofascial pain comes from muscles and fascia, while nerve irritation more commonly causes radiating numbness/tingling. Symptoms can overlap, which is why evaluation matters.
-
Yes. Stress and poor sleep can increase muscle tension and make pain sensitivity worse during flare-ups.
-
Many people improve with coordinated care that restores mobility, strengthens support muscles, and retrains daily movement—often combining PT, chiropractic care, acupuncture, and targeted pain management options when appropriate.
-
For some patients, dry needling can help reduce trigger point sensitivity and improve mobility. We’ll recommend options based on your needs and comfort.
-
Often, no. Some insurance plans require a referral or authorization—if you’re unsure, we can help verify.
Related Resources
Related Conditions
Headaches & TMJ Dysfunction